Osseointegration Quick Links: Overview | Who is a Candidate | Osseointegration Advantage | How It Works | Risks | Recovery | Articles and Links

Meet the Osseointegration Limb Replacement Team of Surgeons
Watch a post-op interview with Dan.
Dog with prosthetic paws inspires Ukrainian veterans recovering from wounds of war
Petra, 17 months after femur osseointegration surgery with Dr. Rozbruch, shares her story
Dr. Rozbruch gives detailed overview of Osseointegration Limb Replacement Surgery
Post-Operative Osseointegration Patient Visit with Dr. Rozbruch
Dr. Rozbruch Presents – Double Above Knee Amputee Wounded Warrior
Dr. Rozbruch explains Osseointegration Limb Replacement using an animation:
Dr. Rozbruch interviewed about osseointegration – part one:
Dr. Rozbruch interviewed about osseointegration – part two:
A brief overview on osseointegration from Dr. Rozbruch:
HSS Minute- Osseointegration Prosthetics for Leg Amputees:
Osseointegration for Short Above the Knee Amputation:
Dr. Rozbruch discusses osseointegration of femur:
Dr. Rozbruch discusses osseointegration in the tibia:
Dr. Rozbruch interviewed by Cyborg4Life Podcast:
More videos:
New! Amputee Osseointegration Surgery Explained at HSS with Dr. Hoellwarth
Soft-tissue Contouring and Nerve Management During Osseointegration Limb Replacement
Back in the Game: Thamer Alatawi’s Story on HSS.edu – See Thamer’s progression of walking through time.
Dr. Rozbruch interviewed about osseointegration limb replacement surgery
Live Tibia Osseointegration Surgery After Primary Amputation
Osseointegration limb replacement patient, Jesse Levine
Randy shows the benefits and advantages of osseointegration
Animation of Tibial Reconstruction Using Osseointegration
When to Amputate and When to Reconstruct a Limb
Two Patients Whose Lives Have Been Changed by Osseointegration
Emily’s Recipe: Stoma Care After Osseointegration
What is Osseointegration?
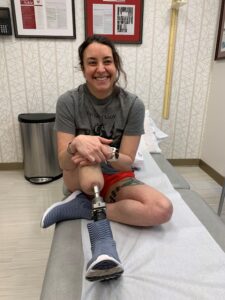
Today, amputation reconstruction specialists at HSS are using osseointegration in limb replacement surgery for amputee patients who have not tolerated or do not want to use a socket. This is a major advance in amputation surgery of both the lower and upper extremities.
Limb replacement surgery
HSS was the first hospital in the United States where osseointegration is being used to treat people who have had transtibial amputations.
Who is a candidate for osseointegration limb replacement?
This type of surgery is especially helpful for amputees who are not doing well with their socket. When the residual limb is short, wide , scarred, or painful, the use of a socket is often fraught with difficulty. Socket problems include pinching, sweating, pain, poor fit, and poor ability to control the prosthetic limb.
What are the advantages over traditional prosthetic limbs?
Bone-anchored prostheses have shown to lead to better patient outcomes than standard, socket-based prostheses. There are many common problems associated with sockets, which an osseointegrated prosthesis can reduce or eliminate. These include:
- Poor fit or need for frequent refitting
- Mobility challenges and lack of patient confidence
- Nerve pain (neuroma)
- Skin sores and ulcers
- Pinching
- Perspiration
Problems in socket prostheses

In traditional prosthetic leg systems, there can be a poor fit between the residual limb and the socket. Many patients experience significant changes in size and shape of their residual limb during the first 12 to 18 months after amputation surgery.
In addition, the angle at which the remaining leg bone rests inside a socket is often, at an angle to the prosthetic leg. This is called malalignment. Such awkward angles can cause balance problems and poor energy transfer. This can make it difficult for patients to move well, and can even lead to falls and fractures.
Other problems associated with point of contact with a socket include sweating, skin irritations or lesions and exacerbated nerve pain. Many amputees experience nerve pain in the residual limb, which is caused by a neuroma . This can be described as “phantom” leg or arm pain. In most cases, wearing a socket puts pressure on the remaining section of the limb, which worsens this nerve pain.
The osseointegration advantage
With osseointegration limb replacement surgery, a custom-made limb prosthesis is directly connected to the skeleton by way of an implant that is aligned with the bone of the residual limb (for example the femur or thighbone, tibia or leg bone, humerus or upper arm bone, radius and ulna or forearm bones). This eliminates all the problems associated with sockets, leading to:
- Improved mobility (for example control of the prosthetic leg)
- Improved proprioception
- Reduced nerve pain
Direct skeletal connection between the prosthesis and the patient’s own bone improves energy transfer, strength and stability. Patients have better control over the prosthetic leg or arm.
In particular, patients who have an osseointegrated prosthetic limb have dramatically improved proprioception, called osseoperception, Touch vibrations to the implant (such as during impact with the ground while walking) can be transferred through to the person’s natural bone. This provides significantly enhanced mechanics, physical stability and energy transfer as compared to standard limb prostheses. The result is that patients feel more connected to the prosthesis not only functionally, but also emotionally. Additionally, individual types of prosthetic limbs designed for different purposes can be easily connected to and disconnected from the implant abutment using an Allen wrench (hex key) or, with some designs, quick-connect hardware.
New surgical procedures to alleviate the pain associated with amputation neuromas can now also be performed together with osseointegration surgery. These include:
- Targeted Muscle Reinnervation (TMR)
- Regenerative Peripheral Nerve Interface (RPNI) with free muscle graft
Improved movement in upper limbs
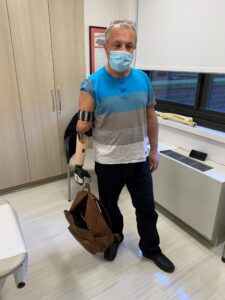
In arm and hand patients, the large harness and socket often used in upper extremity prosthetics is eliminated. This enables the patient to actively use their own body’s natural shoulder and elbow movement.
Osseointegrated arm implants are also compatible with myoelectric prostheses , in which muscle twitches in the residual arm communicate with the arm prosthesis to allow you to actively move your prosthetic elbow, wrist and hand. New technologies use pattern recognition algorithms to relay, in real time, muscle movement signals from the residual limb to your brain and then back to microcontrollers that allow you to control the movement of a bionic (robotic) prosthetic arm or hand. In some cases, TMR is used to enhance the muscle signals.
How does osseointegration surgery work?

The process begins with front- and side-view X-rays and CT scans of your limb to determine precise measurements for your custom-made implant. After we gather measurements, we build a precise custom-made prosthetic implant to fit inside your bone. The implant is then inserted into residual limb bone, and connected to a dual post (AKA dual cone) that, on the other end, connects to a prosthetic limb.
During surgery, we address the neuromas and soft tissues. We perform soft-tissue contouring that usually involves removing, lifting, and tightening excess and loose soft-tissue.
At HSS we have assembled an interdisciplinary team of healthcare practitioners for osseointegration patients. The team effort cannot be underestimated, and each person plays an essential role in ensuring the best outcomes for patients.
- Surgical team (surgeons, anesthesiologists, nurses)
- Prosthetic professionals known as orthotists or prosthetists
- Physical and occupational therapists
What are the risks?
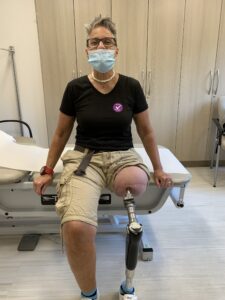
As with any surgery, osseointegration carries with it a risk of infection. However, severe infections, fracture or loosening of the implant are very rare.
If you should fall after receiving your osseointegrated implant, a designated breaking point in a section of the prosthesis will prevent both injury to your bone and damage to the implant. Like ski bindings that release during a fall, the connection between the implant and the prosthesis contains a fail safe mechanism to protect the bone and implant in case of a severe fall
What is the recovery time for osseointegration surgery?
Osseointegration patients can expect to spend an average 3-4 days in the hospital. Generally, our patients are out of bed the next day, when we will apply a rubber footie to the end of the abutment and begin a gradual loading program. A gauze wrap will be applied to the limb abutment for a few weeks and patients can begin a daily shower and cleaning of the stoma with soap and water four days post-surgery.

Gradual loading of weight takes place over several weeks, during which time patients use crutches to prevent from putting full weight on the limb. We start with 20 pounds for 10-15 minutes four to six times per day and increase gradually until the prosthetic leg is attached. In- patient physical therapy begins the day after surgery, and is followed by outpatient therapy once the patient is discharged from the hospital. Prosthetic leg will be attached from three to ten weeks after surgery, depending on bone quality. Patients use crutches for 6 weeks after the leg is attached. The actual growth of bone into the implant takes time, but can be expected about 3 months after surgery.
The total average recovery period – the time by which most patients can be walking without crutches – is approximately three months after surgery.
How long does an osseointegrated prosthesis last?
An osseointegrated prosthesis offers an excellent long-term outcome. This procedure has been performed in Sweden since 1990. The implant lasts for many years after successful osseointegration with the bone although connection parts may need to be changed by the prosthetist. The implant designs improved in recent years and we expect these to function well over decades. The need for revision surgery is possible in cases of fracture, loosening, or deep infection, but complications like this are rare.
Osseointegration Articles, Links, and Publications
Facebook Patient Group – Dr. Rozbruch’s osseointegration patients started a facebook page to share information
Eschen Prosthetics – Osseointegration
Osseointegration Podcast
Articles:
2025
- “Limb Loss Awareness 5K represents a milestone for many,” Brittany Flowers, April 2025
- “He’s Sharing His Osseointegration Surgery on YouTube,” Living with Amplitude, March 2025
2023
- “Mom With Rare Pain Condition to Get Osseointegration Surgery at HSS,” WZZM13 Michigan, December 4, 2023
- Joel Legaweic’s Story, HSS Back in the Game, 2023
- “Constructing an Osseointegrated Prosthetic Leg,” by Haris Kafedzic, MPO, CPO, S. Robert Rozbruch, MD, Taylor J. Reif, MD, Jason S. Hoellwarth, MD, JB&JS
- “Boom times ahead for osseointegration nation?” livingwithamplitude.com, March 2023
2022
- “Osseointegration of the Tibia After a Primary Amputation,” Geiger, Erik J. MD; Hoellwarth, Jason S. MD; Reif, Taylor J. MD; Rozbruch, S. Robert MD, JBJS Essential Surgical Techniques, October-December 2022
- “Revision Amputation with Press-Fit Osseointegration for Transfemoral Amputees,” Hoellwarth, Jason S. MD; Reif, Taylor J. MD; Rozbruch, S. Robert MD, JBJS Essential Surgical Techniques, April-June 2022
- “Medical advances: Limb loss and prosthetic technology,” Wisconsin Public Radio, September 14, 2022
- Jill Gambino’s Story, HSS Back in the Game, 2022
2021
- “Osseointegration Improves Outcomes for Amputees,” HSS Annual Report, 2021
- “Osseointegration Technologies Improve QOL For Leg Amputees,” Orthopedics This Week, October 29, 2021
- “Osseointegration implantation may improve outcomes for lower limb amputees,” Orthopedics Today, October 21, 2021
- “Osseointegration May Yield Improvements for Patients with Transtibial Amputations” Orthopedics Today, August 24, 2021
2018-2020
- “I Got Blown Up in Iraq. Years Later, Amputating My Leg Set Me Free.” Elana Duffy’s story and experience with osseointegration – The New York Times, September 10, 2020
- Featured on NY1, David Giaimo’s quest for a better fitting, more comfortable prostheses led him to Dr. Rozbruch at Hospital for Special Surgery. February 7, 2018
Publications:
- Transcutaneous osseointegration for amputees with short residual bone: Is there increased risk for complications? – A pilot study. J Limb Lengthen Reconstr 2022;8:115-20. Jason Shih Hoellwarth, Adam Daniel Geffner, Taylor J Reif, S Robert Rozbruch.
- Periprosthetic Femur Fractures in Osseointegration Amputees. The Journal of Bone and Joint Surgery Case Connector: July-September 2022 – Volume 12 – Issue 3 – e21.00778. S. Robert Rozbruch, MD and Jason S. Hoellwarth, MD.
- Transfemoral Osseointegration for a Patient with a Very Short Residual Femur After Amputation. S. Robert Rozbruch, MD and Jason S. Hoellwarth, MD. Grand Rounds from HSS: Management of Complex Cases | Volume 11, Issue 2.
- Benefits of osseointegration over socket implants for amputees. ResearchFeatures.com. July 2022. Taylor J. Reif, MD and S. Robert Rozbruch, MD.
- Unexpected positive intraoperative cultures (UPIC) at index osseointegration do not lead to increased postoperative infectious events. J. Bone Joint Infect., Volume 7, Issue 4. Jason S. Hoellwarth, Taylor J. Reif, Michael W. Henry, Andy O. Miller, Austin C. Kaidi, and S. Robert Rozbruch.
- Revision Amputation with Press-Fit Osseointegration for Transfemoral Amputees. JBJS Essential Surgical Techniques: April-June 2022 – Volume 12 – Issue 2 – e21.00068 doi: 10.2106/JBJS.ST.21.00068. Hoellwarth, Jason S. MD, Reif, Taylor J. MD; Rozbruch, S. Robert MD.
- Osseointegration Amputation Reconstruction. Curr Phys Med Rehabil Rep (2022). https://doi.org/10.1007/s40141-022-00344-9. Reif, T.J., Jacobs, D., Fragomen, A.T. et al.
- Attachment of a Myoelectric Prosthesis After Transulnar Osseointegration Implantation. THE JOURNAL OF BONE AND JOINT SURGERY. October-December 2021 – Volume 11 – Issue 4 – e21.00381. Kayla M. Jaime, MS, Taylor J. Reif, MD, Haris Kafedzic, MPO, CPO, Glenn Garrison, LPO, CPO, Jennifer Dhawan, MSOP, MScRS, and S. Robert Rozbruch, MD.
- Osseointegration for Amputees, Current Implants, Techniques and Future Directions. THE JOURNAL OF BONE AND JOINT SURGERY. March 2020 – Volume 8 – Issue 3 – e.0043. Jason Shih Hoellwarth, MD, Kevin Tetsworth, MD, FRACS, S. Robert Rozbruch, MD, M. Brianne Handal, MS, Adam Coughlan, MBBS, Munjed Al Muderis, MBChB.
- Soft Tissue Contouring at the Time of Osseointegrated Implant Reconstruction for Lower Extremity Amputation. Annals of Plastic Surgery. Volume 85, Supplement 1, July 2020. Andrew A. Marano, MD, Omeed Modiri, BS, S Robert Rozbruch, MD, and David M. Otterburn, MD.
- Early Experience with Femoral and Tibia Bone-Anchored Osseointegration Prostheses. THE JOURNAL OF BONE AND JOINT SURGERY. Open Access – e21.00072. Taylor J. Reif, MD, Nathan Khabyeh-Hasbani, BS, Kayla M. Jaime, MS, Gerard A. Sheridan, MCh, FRCS, David M. Otterburn, MD, FACS, and S. Robert Rozbruch, MD, FAAOS.
- Attachment of a Myoelectric Prosthesis After Transulnar Osseointegration Implantation – A 2-Patient Case Study. THE JOURNAL OF BONE AND JOINT SURGERY Case Connector – Volume 11 – Issue 4 – 2021;11:e21.00381. Kayla M. Jaime, MS, Taylor J. Reif, MD, Haris Kafedzic, MPO, CPO, Glenn Garrison, LPO, CPO,
Jennifer Dhawan, MSOP, MScRS, and S. Robert Rozbruch, MD. - Percutaneous Osseointegration Prosthesis. Springer Nature Switzerland AG 2022 265. H. Özger et al. (eds.), Orthopedic Surgical Oncology For Bone Tumors, https://doi.org/10.1007/978-3-030-73327-8_26. Taylor J. Reif, Austin T. Fragomen, and S. Robert Rozbruch.
Limb Lengthening on Instagram: #OsseointegrationStories
Nancy from Boston was struggling with her mobility a few years ago, challenged by severe arthritis of her left knee and a right transtibial amputation. After Osseointegration Limb Replacement Surgery and total knee replacement, she is thriving and very active caring for her granddaughter. #osseointegration #amputee #hssllcrs #hsslimblengthening @hspecialsurgery @limblengtheningreconstruction
Sharon is one of our #osseointegration all stars ⭐️. She put her faith in our Limb Replacement Center to improve her life when her knee was no longer functioning. I’m thrilled she is back to her life with a renewed outlook!
#hssllcrs #hsslimblengthening #orthopedics #orthopedicsurgery @hspecialsurgery
Anthony after Osseointegration Limb Replacement Surgery is doing really well. He could not manage with a socket and now with a bone anchored prosthetic, his mobility has dramatically improved. #osseointegration #amputee #hssllcrs #hsslimblengthening #amputeelife @hspecialsurgery
Dan my Osseointegration Limb Replacement Surgery patient invited me to do the 5 Borough Bike tour 40 miles with him. It was a great day! Dan is an inspiration. He navigated the entire day so well including loading and unloading his bike, walking with bike in crowd, and riding 40 miles. #osseointegration #hssllcrs #hsslimblengthening #amputee
David age 69 from Atlanta, Georgia had been an #amputee for 47 years. 10 weeks postop single stage Osseointegration Limb Replacement Surgery he is walking on his new leg. #osseointegration #hssllcrs #hsslimblengthening @hspecialsurgery
Last week I lectured at the International Society of Orthopedic Centers (ISOC) meeting of the world’s top 20 orthopedic surgery centers in the Netherlands. topic was Osseointegration Limb Replacement Surgery. Great symposium with my Dutch colleagues @robinatallah who have a substantial experience. Great representation from many @hspecialsurgery colleagues. Wonderful country and I visited Amsterdam, Utrecht and Arnhem experiencing museums and the Dutch masters, a lot of bicycles, windmills, tulips, canals, Dutch beer and pancakes. #hssllcrs #hsslimblengthening #osseointegratıon #amputee
Susan had a painful knee replacement for many years that was draining pus and was stiff and limited her mobility. She had failed revision knee replacement and was offered nothing else. Just a few months after Osseointegration limb replacement mobility has improved dramatically as well as her quality of life. #osseointegratıon #amputee #hssllcrs #hsslimblengthening
Jason 4 months post Osseointegration Limb Replacement Surgery. After trauma years ago, he has been living with a chronic painful dysfunctional limb that limited his life. #amputation reconstruction provided new hope. #osseointegration #hssllcrs #hsslimblengthening @almorthoinc @hspecialsurgery



